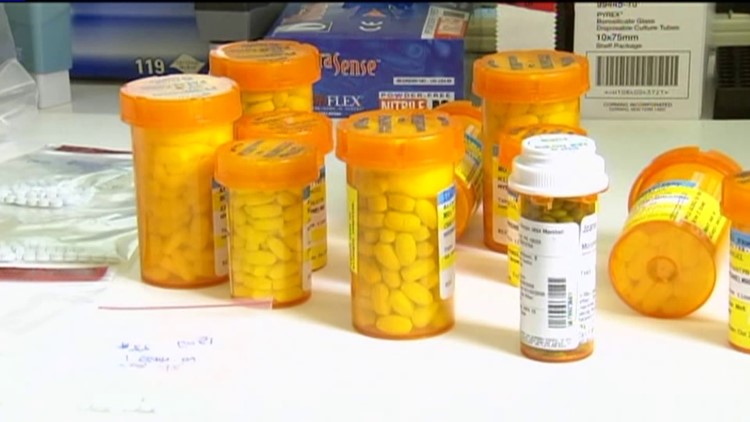
Earlier this month the State Comptroller Kevin Lembo and the Connecticut State Medical Society hosted a forum on soaring drug prices and pharmacist, Dr. Michael White from the UConn School of Pharmacy was one of the panelists along with representatives from the pharmaceutical industry and a leading pharmacy benefit managing company.
The expense of prescription drugs are very expensive and directly impacts the pocketbooks of seniors, people with chronic disease, businesses, and the state and federal government. $374 billion is currently spent annually on prescription drugs and in 2014 costs rose by 13%, the greatest increase since 2001, before going back to a more sustainable increase last year. One area responsible for 73% of the growth in drug spending over the past 5-years are biologic drugs, also known as specialty drugs. These drugs have brought about major new therapies for cancer, Hepatitis C, multiple sclerosis, rheumatoid arthritis, and orphan diseases which only affect a few hundred or thousand people and up to now had no effective therapies. However, the average yearly cost of a biologic drug is $53,000, higher than the median US household income and three times the Social Security retirement benefit.
Bringing a new drug to market is very expensive, especially biologic drugs that are being developed for a relatively small number of patients. So cost recuperation is spread over several thousand people instead of hundreds of thousands of people. Having said that, pharmaceutical companies are not charities, they are trying to beat market expectations. We don’t want a drug industry that cannot make a profit because this was the reality in the generic drug market for years and it led to tremendous consolidation in the industry and has resulted in fewer choices, more drug shortages, and ultimately rising prices. The secret is to incentivize innovation so we can improve patient health without bankrupting the system and that is not easy to do because it requires making hard choices that reduce accessibility.
The FDA recently released rules for creating biosimilars which will be like generic medications for biologic drugs. While there are only two biosimilar drugs FDA approved, it is estimated that they could save the US $44 billion by 2024 when a large number of biologic drugs lose patent protection. Connecticut needs a biosimilar law to allow greater use of these less expensive but similar alternatives. Secondly, we should not have direct to consumer advertising, companies spending on direct to consumer advertising rose 30% over the past two years because they increase use of brand name medications. Only New Zealand and the US allow it and the American Medical Association has called for it to stop. I agree, these decisions should be made based on the evidence, not name recognition. Third, we need more comparative effectiveness research so that doctors, insurers, and patients can understand where a drug offers a clear advantage over other options and where the benefits are poorly substantiated so we can make reasonable choices of where to spend our healthcare dollars. This ties into the use of tiered formularies, prior authorization, and step therapy which are inconvenient for patients and burdensome for doctors but is the only effective way to target who can receive a medication and create competition in the marketplace to hold down costs. If a company knows that you will choose one drug in the class to be preferred and that people won’t be able to use their drug if the cost is too high, costs will go down. If people can receive a Cadillac drug for the same price as a Hyundai, they will of course want the Cadillac drug. It is just human nature. We need market forces and competition to influence healthcare decisions but only when there are viable alternatives so that we are not resorting to rationing.
Dr. Michael White, UConn School of Pharmacy